-
Case Study: Algorithms for Diagnosing TB
[activity type]
Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in using the Algorithms for Diagnosing TB. Choose which case study you would like to review (but do not share this with the mentee).
-
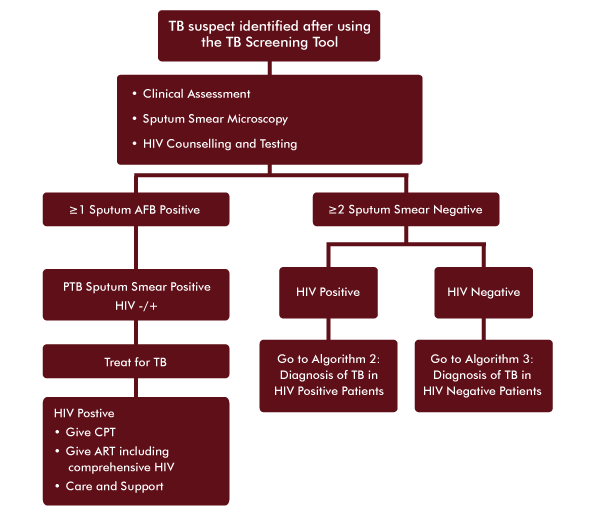
 Presumptive TB Case- HIV Status Unknown
Presumptive TB Case- HIV Status Unknown -
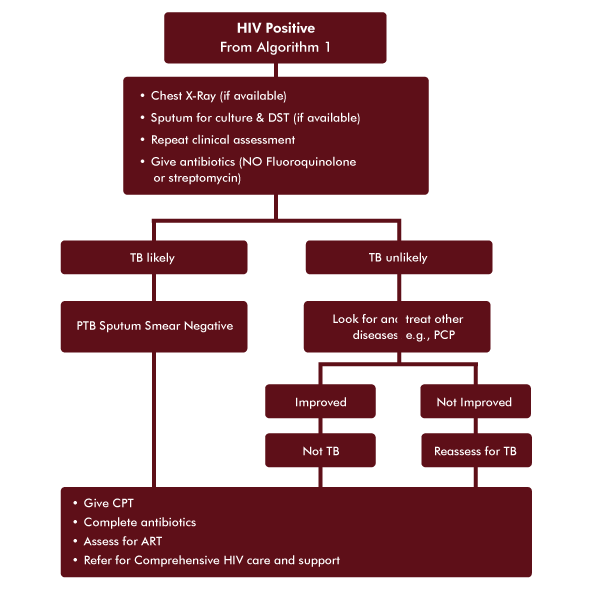
 HIV Positive Sputum Smear Negative Patient
HIV Positive Sputum Smear Negative Patient -
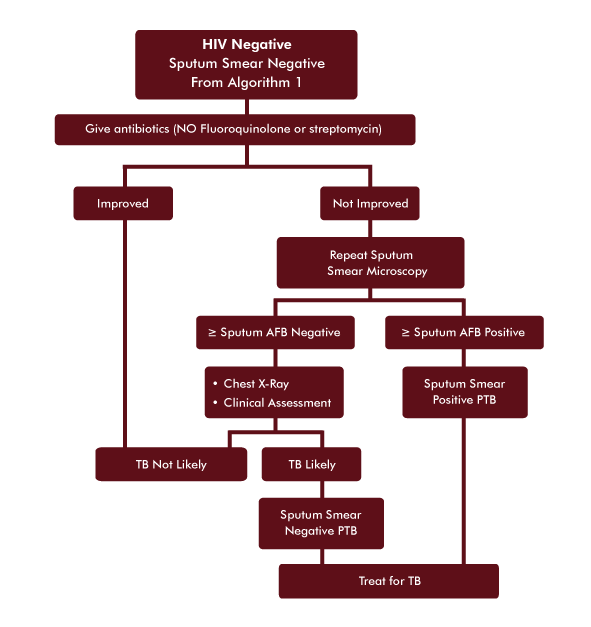
 HIV Negative Sputum Smear Negative Patient
HIV Negative Sputum Smear Negative Patient
Case Study 1
Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in using the Algorithm for the Diagnosis of TB in A Presumptive TB Case with Unknown HIV Status.
Zinyoro is a 20-year-old male student presenting in your clinic with a cough and weight loss for the past month. He tells you he thinks he is sick from staying up late studying for exams. He does not report any medical problems in the past. He does not know his HIV status.
Vital signs: Temperature: 36.3 C, HR: 82 and regular, RR: 20, B/P 123/78, Weight 73kg
Physical exam: Chest exam reveals right-sided anterior crackles
-
What are your next steps in evaluating Zinyoro’s symptoms?
- Use the TB screening tool to further evaluate his risk for TB.
- Ask about HIV status and if not known, provide pre-counseling and HTC.
- Obtain spot sputum specimen and send to the laboratory immediately.
- Provide patient education with each step of the evaluation.
- Ask about TB contact.
Additional Information
Zinyoro’s spot sputum is negative and his HIV test is positive. When you tell him the results, he is visibly shaken and upset and tells you that the results must be wrong.-
What are your next steps in evaluating Zinyoro’s symptoms?
- Provide counseling and psychosocial support. Ensure patient understands information being given and allow for sufficient time for questions.
- Proceed to Algorithm for Diagnosis of TB in HIV Positive Smear Negative Patient.
- Give him a chest X-ray (if available).
- Get a sputum for culture and DST (if available).
- Perform a complete physical examination, if not already done, focusing on HIV related signs and symptoms such as enlarged lymph nodes and oral candidiasis.
- Get HIV baseline laboratory tests.
- Give an antibiotic but not a Fluoroquinolone or streptomycin. Amoxicillin for 5 days is one option. Close follow-up is needed to evaluate for improvement. If there is improvement, this would suggest that he may have PCP, bacterial pneumonia, or another respiratory condition; although TB should remain one of your differential diagnoses. It is important that the patient is closely monitored and returns to the clinic to be re-evaluated after antibiotics or sooner if his condition worsens.
- Refer for comprehensive HIV care and support.
-
What will you do if Zinyoro returns after completing the course of antibiotics without improvement?
- Assess further to rule out other potential diagnoses. If no improvement or continued worsening, reassess for possible TB.
- Initiate CPT unless this has been started at the HIV clinic.
- Coordinate TB care and treatment (if initiated) with initiation of ART.
Case Study 2
Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in using the Algorithm for the Diagnosis of TB in HIV Positive Sputum Smear Negative Patient.
Anele is a 31-year-old female diagnosed with HIV infection 2 years ago. She presents today with a fever and cough of 2-3 weeks duration. She also tells you that she thinks she has lost some weight but is not sure. She has no previous history of TB. She takes an herbal drink given to her by her mother “to keep her healthy” and occasionally paracetamol when her feet hurt after standing at her work. She disclosed her HIV status to her mother, who she lives with along with her grandmother. She tells you that her grandmother has been coughing but refuses to go to the clinic.
Vital signs: Temperature: 37.6 C, HR: 63 and regular, RR: 18 B/P 118/76
Physical exam: Unremarkable except for a small (1cm) submandibular lymph node on the right side
-
What is the next step in the evaluation of this patient?
- Collect spot sputum specimen and instruct patient to obtain second specimen in the morning and bring it to the laboratory immediately. If unable to come back to the clinic, have Anele wait for 2 hours and collect the second specimen.
- Get a chest x-ray (if available).
Additional Information
The spot sputum specimen is positive.-
Discuss the management of Anele now that she has a positive sputum specimen and is HIV positive.
- Obtain sputum for culture and DST (if available).
- Get chest x-ray (if available).
- Treat for TB.
- Begin CPT unless she is already taking this.
- Do contact tracing.
- Refer for comprehensive HIV care and treatment unless she is already being seen in that clinic.
- Initiate ART when tolerating TB treatment but at least 2 weeks after the start of TB treatment (Zimbabwe ART Guidelines 2013).
- Get a baseline CD4 count.
- Discourage the herbal drink because some herbs interact with medications by either increasing/slowing metabolism. This interaction alters the plasma concentration, which has an effect on the optimal therapeutic drug levels.
Case Study 3
Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in using the Algorithm for the Diagnosis of TB in HIV Negative Initially Sputum Smear Negative Patients.
Bukhosi is a 42-year-old man complaining of a productive cough and fatigue for 2 months. He is complaining of weight loss. He tells you that his wife was treated for TB in the past but he does not know if she finished her medication. She went to live with her mother and took their 2 children.
Vital signs: Temperature: 38.0 C, HR: 100, RR: 18, B/P 118/70, Weight: 70 kg
Bukhosi is thin and breathing comfortably.Physical exam: Chest exam reveals fine crackles in all lung fields.
HIV test is negative. Spot sputum smear is negative.-
What would be the next steps in evaluating this patient?
- Collect spot sample of sputum and send to the laboratory immediately.
Additional Information
Bukhosi’s spot sputum specimen is negative. You explain that a second specimen is needed to make sure that he does not have TB. The specimen should be taken tomorrow morning and brought to the laboratory. Bukhosi tells you that he lives too far from the clinic and cannot return tomorrow. He is also afraid that if he does not go to work, his boss will be very angry and he could lose his job.-
Do you need a second specimen? If so, how will you obtain the second sputum specimen?
- Yes. Have Bukhosi wait 2 hours and collect a second specimen today.
Additional Information
Bukhosi’s second specimen is also negative.-
What is the next step in managing this patient?
- He is HIV-negative and has no danger signs (unable to walk unaided, respiratory rate 30 or more, T>39.0, pulse>120).
- He should be treated with antibiotics but not a Fluoroquinolone or streptomycin. Amoxicillin for 5 days is one option. Close follow-up is needed to evaluate for improvement.
- If there is improvement, his would suggest that he may have bacterial pneumonia or another respiratory condition, although TB should remain one of your differential diagnoses. It is important that the patient is closely monitored and returns to the clinic to be re-evaluated after antibiotics.
Additional Information
Bukhosi takes the 5 day course of amoxicillin and returns to your clinic. He is still having a cough and fatigue. The vital signs and exam are not significantly changed from the last visit.-
What is the next step in evaluating this patient?
- Repeat sputum smear microscopy. If negative, check chest x-ray (if available).
- Refer for further evaluation as patient is not responding to treatment.
-
If Bukhosi’s chest X-ray results indicate TB disease what is his diagnosis and what else will you do as part of follow-up for this patient’s family?
- Diagnosis is Sputum smear negative pulmonary TB
- Contact screening for all family, household, and community members in close contact with patient.
- Treat any family members who show evidence of TB disease.
-
-
Case Study: Diagnostic Algorithms
[activity type]
Instructions: Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in using the TB diagnostic algorithms.
A 30-year-old HIV-positive man complains of a cough that has lasted for 1 week. He reports purulent expectoration, chest pain, shortness of breath, and chills last night. He was evaluated for ART initiation approximately 6 months ago but his CD4 count was 554 and was told he was not eligible. He was due for a follow-up CD4 count when he became sick.
Ask your mentee:
-
What else do you want to know?
Patient medical and surgical history, current medications including non-prescription, herbs and vitamins, HIV care and treatment linkage (where is he getting his HIV care), adherence to care (clinic/counseling appointments) and treatment (ART, CPT), disclosure, HIV status of partner and children, physical examination, and whether he is in need of urgent care.
-
What will you think about?
Think first of a bacterial pneumonia (sudden onset, short duration). Also TB.
-
In thinking about differential diagnoses, what diagnoses do you consider related to duration of cough?
If lasts days: bacterial pneumonia. If lasts weeks: TB/PCP (pnuemocyctis caranii pneumonia).
-
In thinking about differential diagnoses, what diagnoses do you consider related to sputum production?
- Usually purulent is TB/BP (bacteria pneumonia).
- Dry/scant: PCP/early bacterial pneumonia.
-
In thinking about differential diagnoses, what diagnoses do you consider related to fever quality?
- Common, 39 degrees Celsius or more: think about bacterial pneumonia.
- Low-grade/afebrile: think of TB / PCP.
-
How will you confirm your diagnosis?
- Through chest examination (which may include a chest x-ray), FBC, and AFB taken if possible.
- Urine m/c/s.
- Malaria test.
- Stool m/c/s or rectal swab/blood culture if the temp fails to respond to the treatment.
-
What else do you want to know?
-
Case Study: DR-TB
[activity type]
Tell your mentee that you will review a case study and ask some questions to help him/her improve skills in diagnosing TB.
Maiba is a 44-year-old woman who presented to the clinic 3 months ago with a chronic productive cough, fever, and weight loss. She had recently moved to the village to be near her mother. Maiba informed you that she was treated for TB which had been diagnosed based on positive sputum results one year prior to arriving here and it was managed on the RZHE regimen. Her HIV test was negative a year ago and repeated prior to beginning this current regimen and the HIV test remained negative. Her sputum results tested positive. She was classified as Previously Treated TB case/Relapse and was started on 2(RHZE)S/1(RHZE) daily. For the past 3 months, she was supervised closely by DOT in the clinic and by her mother, who is her treatment supporter. Maiba's adherence has been good, despite continued GI complaints of nausea and poor appetite. She has only gained a small amount of weight even with her mother cooking for her and encouraging her to eat small frequent meals. Today’s visit is the end of her 3-month intensive phase.
Ask your mentee:
-
What will be included in your monitoring visit today?
Vital signs, weight, clinical evaluation including assessment of lung sounds, adherence assessment. Spot sputum examination.
Additional Information
Maiba’s spot sputum was positive.-
What are the next steps needed in this case?
Take sputum for culture and DST and commence continuation phase in consultation with your clinical mentor or HO while awaiting the results of the sputum test. Consultation will be needed with the regional MDR TB team when the results of the DST are available. The continuation phase is started if the sputum specimen is negative or positive.
Note that if the sputum result remains positive after 4 months, all medicines should be stopped for three days and a sputum specimen sent to the National Reference Laboratory for culture and sensitivity. The continuation phase can then be continued. -
Maiba is at risk for drug-resistant TB (DR-TB), which may be due to a number of factors. Give an example of a health worker related factor, health system related factor, and patient related factor.
Health worker related factors- Lack of TB management knowledge
- Inappropriate use of guidelines for the management of TB cases
- Non-compliance with the national treatment guidelines
- Inadequate monitoring of patients on anti-TB treatment
Health system related factors
- Poor quality anti-TB medicines
- Poor storage conditions
- Stock outs
- Absence of clear guidelines
- Poor or inadequately trained healthcare workers
Patient related factors
- Poor adherence
- Difficulty accessing the health facility
- Side effects
- Substance use with failure to adhere to treatment
- Exposure to a DR-TB case
- Immunosuppression
-
What will be included in your monitoring visit today?
-
Role Play: Diagnostic Skills
[activity type]
Explain to the mentee that you are going to engage in a role play to help him or her learn how to improve TB diagnostic skills. He or she will play the role of health care provider and you will be the patient.
Part 1
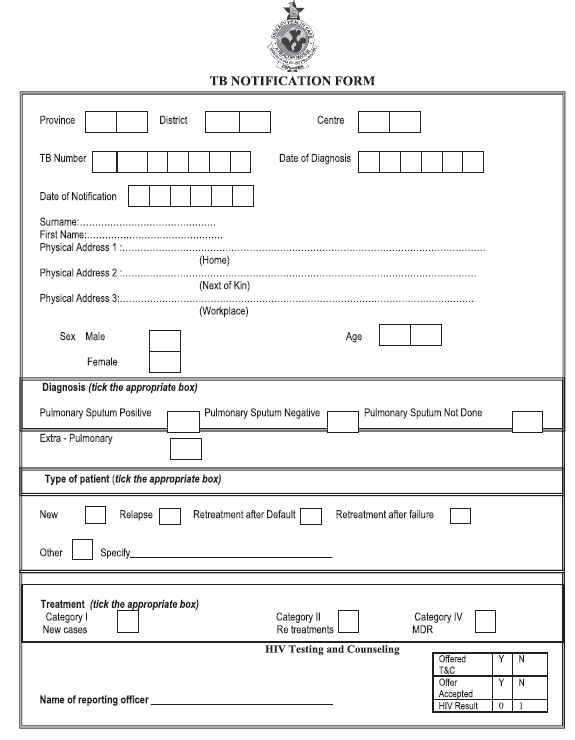
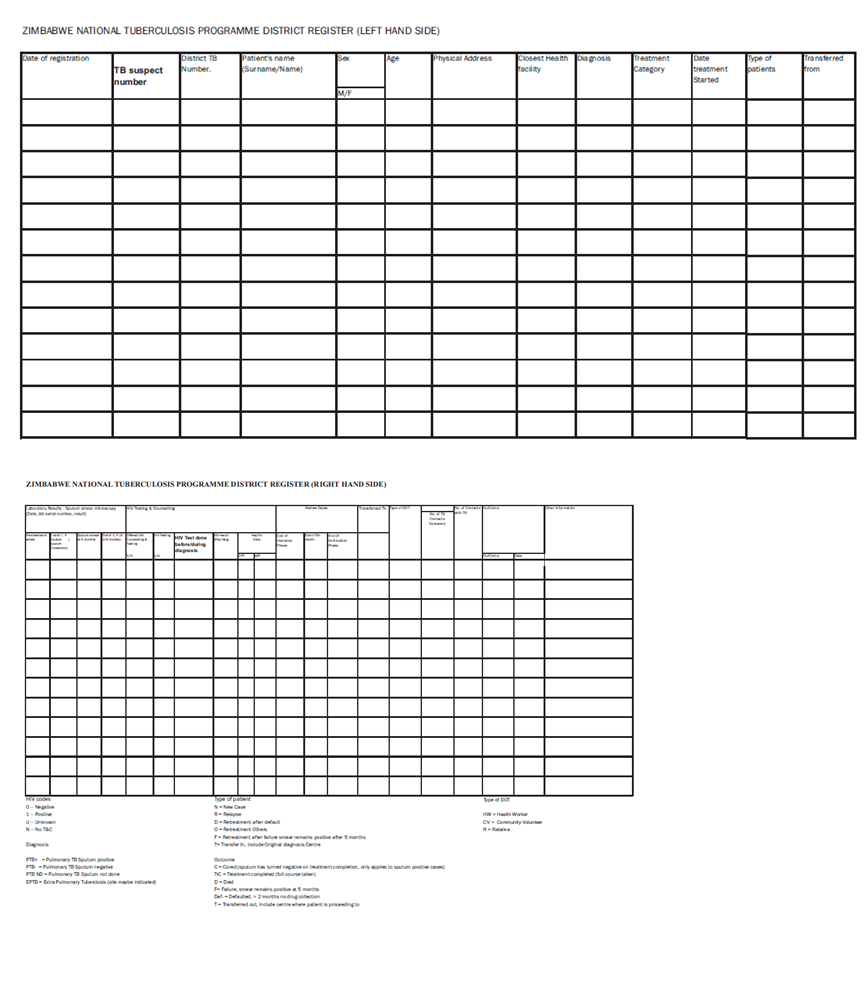
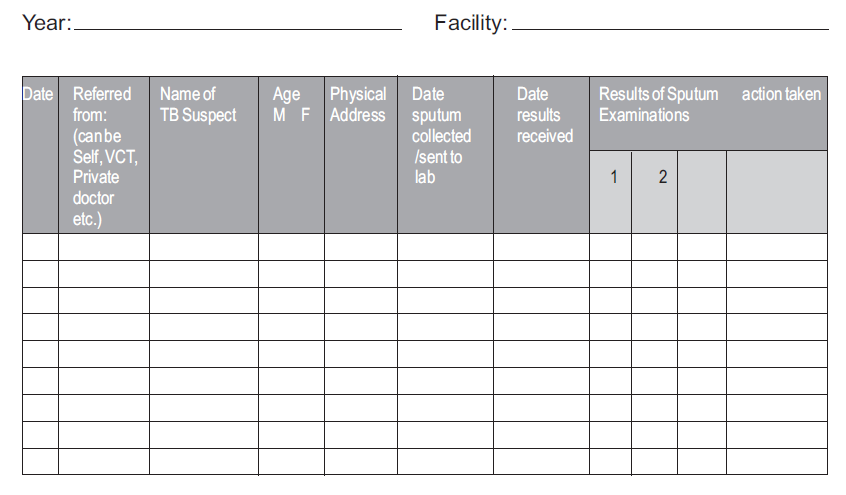
A 26-year-old man has come to the health facility alone. He’s married to Sipiwe and has a 6-month-old child who is breastfeeding. Sipiwe delivered at home because the family could not afford to pay for ANC services. Both are unemployed and stay in a small, one room apartment. The man has been losing weight and has had an irritating, productive cough, especially in the mornings, for the past one month. Ensure that you complete the Presumptive TB Case Register and TB notification form.-
Patient instructions (mentor). Do not show this to the mentee.
Your task is to act the role of this TB patient. You have not been feeling well for several weeks but you have not told your wife. You do not want her to worry since she is taking care of your child and is worried that you have not found work. Sipiwe is your only partner now. You have had many partners in the past, but none were ever sick and you have never had an HIV test.
Your job is to listen carefully during the role play so that you can comment on what was done well and what could be improved.
Check the boxes below to indicate whether the mentee asked the appropriate questions. At the end of the role play, review any problem areas with the mentee.
Part 2
He returns 3 days later. The results of his visit are:
Sputum: Sputum results show no AAFBs but the comment on the results slip says the sputum was salivary.
Still coughing
Temperature: 38.9 degrees Celcius
-
Patient instructions (mentor). Do not show this to the mentee.
You ask the health care provider:
- Do I have TB? Why do I have to give you more sputum? Does the laboratory know how to do the test?
- If I do have TB, have I given that to my child and wife?
- I do not believe that I am HIV positive. Please do the test again now.
Your job is to listen carefully during the role play so that you can comment on what was done well and what could be improved.
Check the boxes below to indicate whether the mentee asked the appropriate questions. At the end of the role play, review any problem areas with the mentee.
-
TB/HIV Co-Infection: Diagnosis
Learning Objective:
- Conduct proper diagnostic tests on presumptive TB cases using the clinical algorithm.
-
Assessment
Observation
Tell your mentee you would like to assess his/her knowledge related to following the proper diagnostic algorithm in 3 different kinds of patients by observing him/her. Inform your mentee that the purpose of this activity is to support him/her in his/her learning and guide them in how he/she can improve his/her practice.
Tap on the type of patient to see the observation checklist. Eventually, try to cover all three of the patient types with your mentee.
Following the observation, provide feedback to your mentee and give mentorship as needed.
-
 Presumptive TB Case- HIV Status Unknown
Presumptive TB Case- HIV Status Unknown -
 HIV Positive Sputum Smear Negative Patient
HIV Positive Sputum Smear Negative Patient -
 HIV Negative Sputum Smear Negative Patient
HIV Negative Sputum Smear Negative Patient
Observation Checklist: Presumptive TB Case- HIV Status Unknown
If you cannot follow up on the patient’s results, ask the mentee what he/she would do…
- If ≥1 sputum AFB is positive, what would you do?
- If ≥2 sputum smears are negative, what would you do?
Observation Checklist: HIV Positive Sputum Smear Negative Patient
If he/she cannot follow up on the patient’s results, ask the mentee what they would do if…
- A PTB sputum smear resulted in a negative?
- He/she suspected other diseases, e.g., PCP?
Ask mentee, if evaluated and treated for PCP with no improvement, what would you do next?
Observation Checklist: HIV Negative Sputum Smear Negative
-
-
Activities
-
Mentor Resources