By conventional standards, Joshua Koopman’s path to the medical field might be considered unusual. His background prior to healthcare was music and visual arts. Joshua was already eight years into his job as a nurse tech at the UW Medical Center on the inpatient physical rehabilitation unit when he took a 4-month break to study abroad in Rome and finish his art degree in painting and print-making. He also plays the guitar and banjo.
“People would say to me all the time, ‘Oh, it’s a good thing you got your arts degree’,” he says with some annoyance. “Because now I’m working in healthcare, and the implication is that I wasted my educational efforts studying art.”
To Joshua’s way of thinking, his arts training paved the way for his future career as a physician assistant. The first indication came at the age of 22 in his hometown of Normal, Illinois. The local hospital was looking for a telemetry monitor. Joshua’s mother, who worked in human resources for that hospital, recommended him to the job.
“Her understanding was, if you can read music, you can read a cardiac telemetry monitor,” he recalls. Joshua applied, was interviewed and hired. “I took a class on how to read rhythm strips and then started monitoring telemetry. I went from delivering pizzas to doing that.”
Joshua was fascinated as he learned about how the heart conduction system worked, and how to interpret it by viewing activity on a monitor. He worked as a telemetry monitor from 2004 until 2007.
Today, as he reflects on the wider impact of his degree in visual arts, Joshua attributes much of it to a greater sense of discipline.
“You have to be able to go into the studio for four, five, six hours a day after classes,” he says. “No one’s going to make you do it. You have to be able to sit down, alone with your work. There’s a lot of critical thinking. You have something that you want to express, or you have some particular image that you want to render, or something you want to do, and you have to figure out how to do it. There’s not a blueprint for those kinds of things in the art world.”
“To me, visual arts, in a lot of ways, is problem solving. I think that’s true in medicine too. You have to take this chief complaint – this collection of symptoms – piece together this picture and figure out what’s going on with this person. You also have to figure out how to listen and sit down with the patient and actually give attention to them. I think there’s a lot of that in the visual arts, too.”
Joshua pauses for a moment, then concludes. “It’s always frustrating to me when people imply that there’s no cross connection. The connection is never ending.”
Growing up with a parent who worked in healthcare administration, Joshua developed a comfort level around hospitals early on. “Anytime I would go to visit my mom, I’d have to go to the hospital to see her,” he recalls. This early exposure had a lot to do with his willingness to look for jobs in the medical field as he grew older.
His interest in medicine grew while working as a telemetry monitor. All of his coworkers were either EMTs, nurse techs or nurses, so Joshua decided to enroll in an Emergency Medical Tech class at the local community college in Normal.
After completing the EMT course, there weren’t a lot of channels to work on ambulances in his home town. “There were a couple of fire department stations, but they didn’t hire too many people,” Joshua says. “The rest was all voluntary.” And so, he looked to the ER and was offered a position at the very hospital where he had been working. “I started working dual roles: as a nurse tech on the floor with patients, and as a telemetry monitor from 2004 to 2007, until I moved to Seattle.”
During this period, Joshua’s skills set broadened as he would float between the ICU, ICU stepdown and the cardiology units.
“It was wonderful,” he says. “It was different going to ICU, cardiac and stepdown. There would be cardiac patients, but then you’d also see all kinds of other things—diabetic patients, patients with hepatitis and liver disease, all kinds of acute illness. There was a lot of variety and it’s still my favorite time in healthcare, the most fun.”
It was also the first time that Joshua realized that there’s a high level of cooperation between staff and teams in healthcare.
“Having worked in jobs like food service before, a lot of people have self-serving agendas,” he says. “People’s health isn’t on the line, and so there’s less motivation to really work together. But when you go into an ICU and someone’s post-op and they are acutely ill, then you have all these people that come together. The task that needs to get done can’t get done unless all of these people agree to do whatever is necessary, and work together. That synergy is amazing to me. It’s one of the biggest drives for me to keep going with healthcare.”
In 2005, Joshua moved to Chicago to attend a school for music and visual arts. Still, he’d make the two-hour drive back to Normal on weekends to work at his hospital job. During this period, he met his wife in Chicago and, after a few years, they were looking to leave the city. “It was a little too big for me,” Joshua says.
His wife’s mother was a professor at Seattle University, and her father worked at UW Medical Center on the inpatient physical rehab unit. So even before Joshua and his wife had moved to Seattle in late 2007, he had procured a job on that unit as a nurse tech and she had free tuition at SU.
“Our resources just kind of pulled us out here to Seattle,” he says. “I had never been here before we moved.”
The inpatient physical rehab unit at the University of Washington Medical Center exposed Joshua to a lot of spinal cord injuries and brain tumors, heart transplants, lung transplants, stem cell transplants and liver transplants. “We didn’t really get the orthopedic patients unless something went wrong,” he says.
The new job required that Joshua learn an entirely new set of skills.
“You know, traumatic brain injuries are totally different than somebody who just got out of open heart surgery. In some ways, it’s easier, and in other ways more challenging. For instance, there’s a lot of confusion with traumatic brain injury. You have to be with them. They have to be under constant observation where you’re just with that one patient all the time, because if they’re left on their own, they’re going to get into trouble. Some patients can be very taxing. They can be emotional, mean, nice, they can sleep all day, or they can be up. There’s a lot of cognitive deficits. Whereas, with a cardiac patient, it’s basically: Are their tubes looking good? Are their vitals good? We need to go for a walk, are you using your incentive spirometer? And so, yeah, I had to learn different skills.”
After eight years in this healthcare role, Joshua began considering that his path forward might include graduate school, but there were certain things that he was looking for. His interests included medicine, music and Buddhism.
“I wanted to be able to have a spiritual component, a human component, and a creative component. I wanted to be able to dig into a particular subject and know it really well.”
Initially, Joshua considered a private Buddhist seminary school in Colorado. He did all the preparatory work was admitted. But the price tag was prohibitive, so he deferred for a year to see if he could get some kind of financial aid, or at least figure out the routes towards employment afterwards that would allow him to pay for his graduate education.
“You know, I could work as a chaplain in hospital, but I would never be able to afford any of my debts,” he concluded.
During his year of deferment, Joshua decided to do his science courses including anatomy and physiology. “I didn’t get any of those with the art degree,” he says. From there an alternate plan developed.
“If, at the one-year point, I do well in the science courses and continue to be motivated, and if I don’t have the money to go to seminary, then I’ll look at these other avenues.”
Joshua spent the year taking A&P, chemistry and other science courses. Finally, he could not defer his admission to the Colorado program any further, and a decision had to be made. “Well, I still really like medicine, and I still really can’t afford seminary. So, I let it go.”
Which was scary for Joshua, as there were no guarantees of getting into PA school.
Physician assistant had come up on his radar because of he had come to know some PAs during his time working in hospitals. “They were so good and I had some friends that did it,” he says. “But it just seemed like a lot.” Joshua did informational interviews with some medical professionals that he knew in order to gauge whether or not a career as a PA was realistically within reach. There was a moment where he realized, “Okay, I just have another year of classes and then I can start this application, and it’s not actually that far away.”
Joshua applied to three PA programs including two on the East Coast. He was invited to interview by all three, was accepted at two, but he selected MEDEX Northwest. “I was already living and working in Seattle. Also, MEDEX was less expensive than those East Coast schools. And MEDEX also has such a wonderful reputation in the PA world.”
Now a part of MEDEX Seattle Class 50, Joshua describes his classmates as amazing people. “It was very intimidating, especially when we did our “Each One Teach One.”
Here, Joshua is referring to an early didactic classroom activity where each student does a presentation on their lives, complete with personal photos. “It was one just insane story after another insane story. I was like, ‘Man, these people are amazing, they’re all world travelers, they’re all so intelligent.’”
Now in his clinical year, Joshua declares his past didactic year at MEDEX as “extremely rewarding, educational and difficult”.
“I tend to over pursue discipline because early on I developed a fear of not succeeding in school,” he says. “I didn’t graduate high school and didn’t do well early in school, and so my entire college career was about gaining more confidence. I still err on the side of caution where I’m very controlled in my environment. You can ask my wife, she’ll tell you all about it.”
We all have our own learning style, and Joshua has developed his out of a unique blend of insecurity, strength, visualization and drive.
“I’m kind of slow,” he explains. “I have to hand write things, I have to type things. I still have sketchbooks full of my anatomy drawings. And I have to do it repetitively. I can’t just look at something once and remember it, especially if I just read it. And I am a textbook reader. I’m probably the only one in our class of 52 that has read all of our textbooks. I have to write stuff down in different formats, so I have quizlets, I have mind maps, I have handwritten notes and pictures. It’s time-consuming, so I was pretty much always going. I won’t acclimate right away to new situations but once I kind of make the adaptation, then I’m fine. And I can take something pretty far, but it just takes me maybe three times. But once I get it, I got it.”

Joshua Koopman prepares to draw blood from a classmate during his MEDEX didactic year IV workshop. Advising is Marc Hawkins, PA-C, MPAS, Associate Program Director.
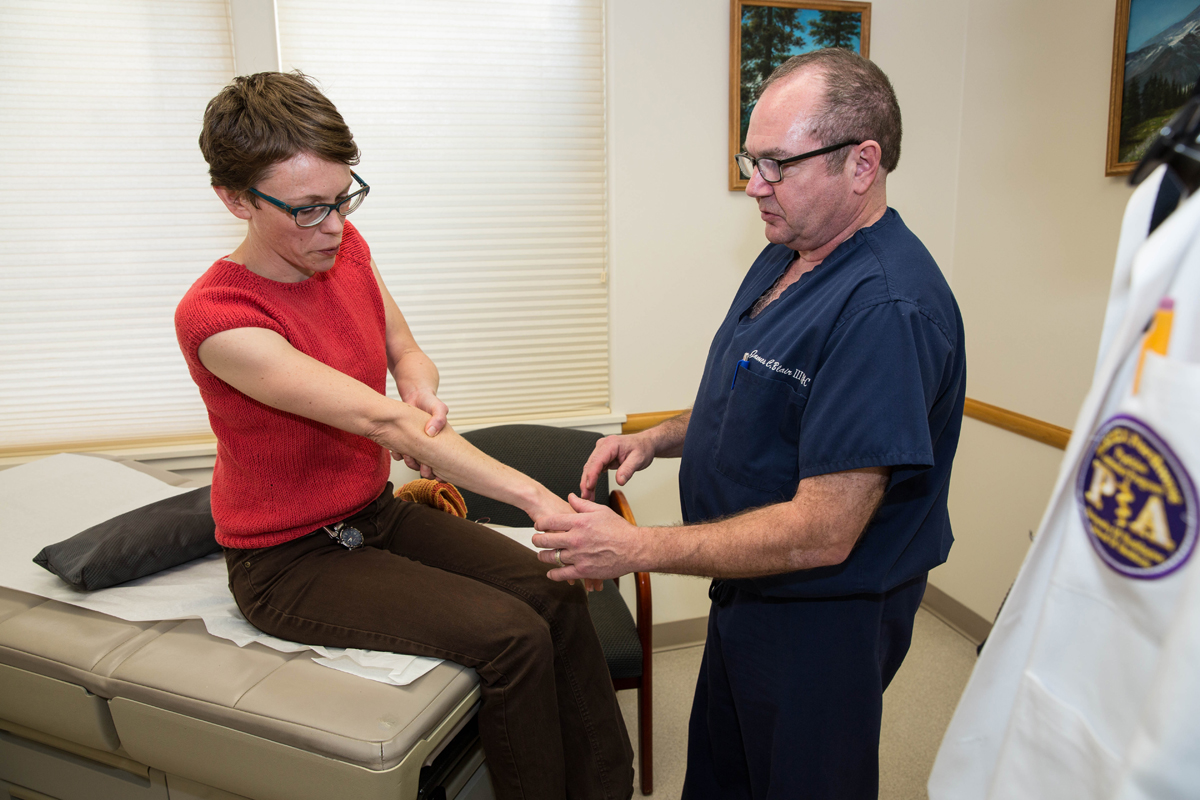
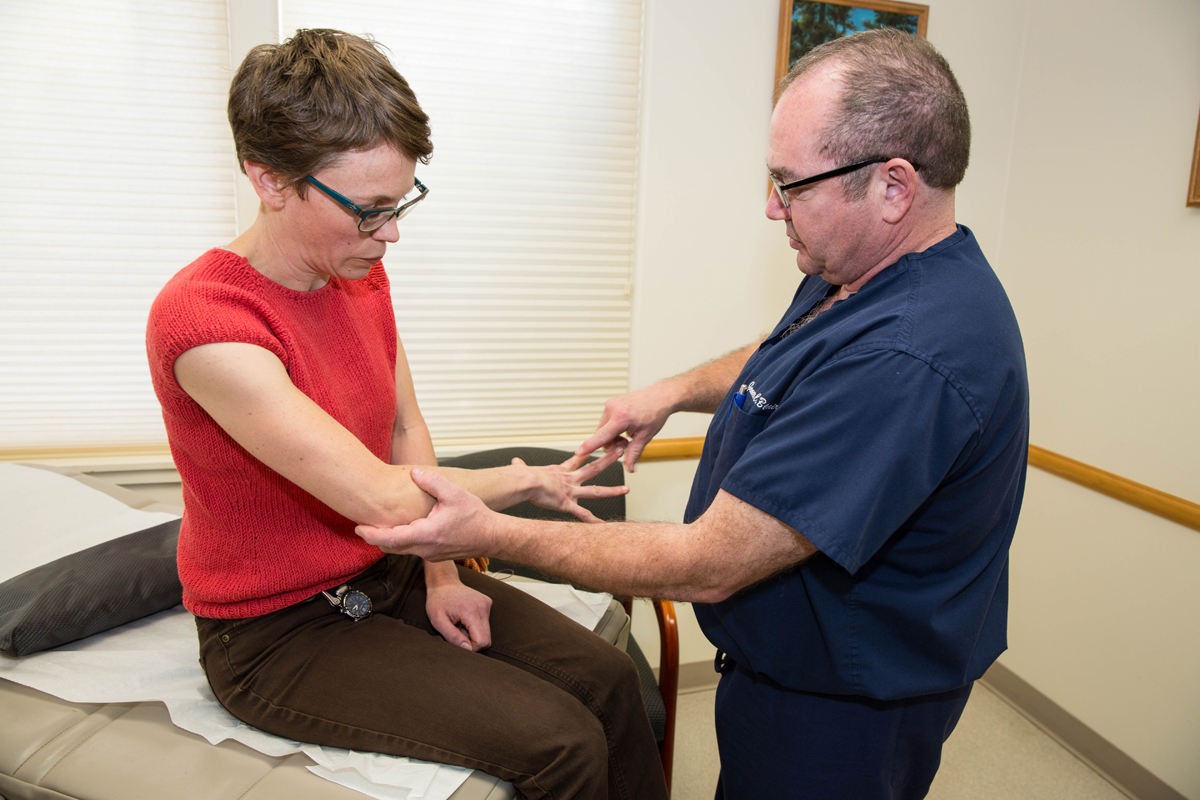
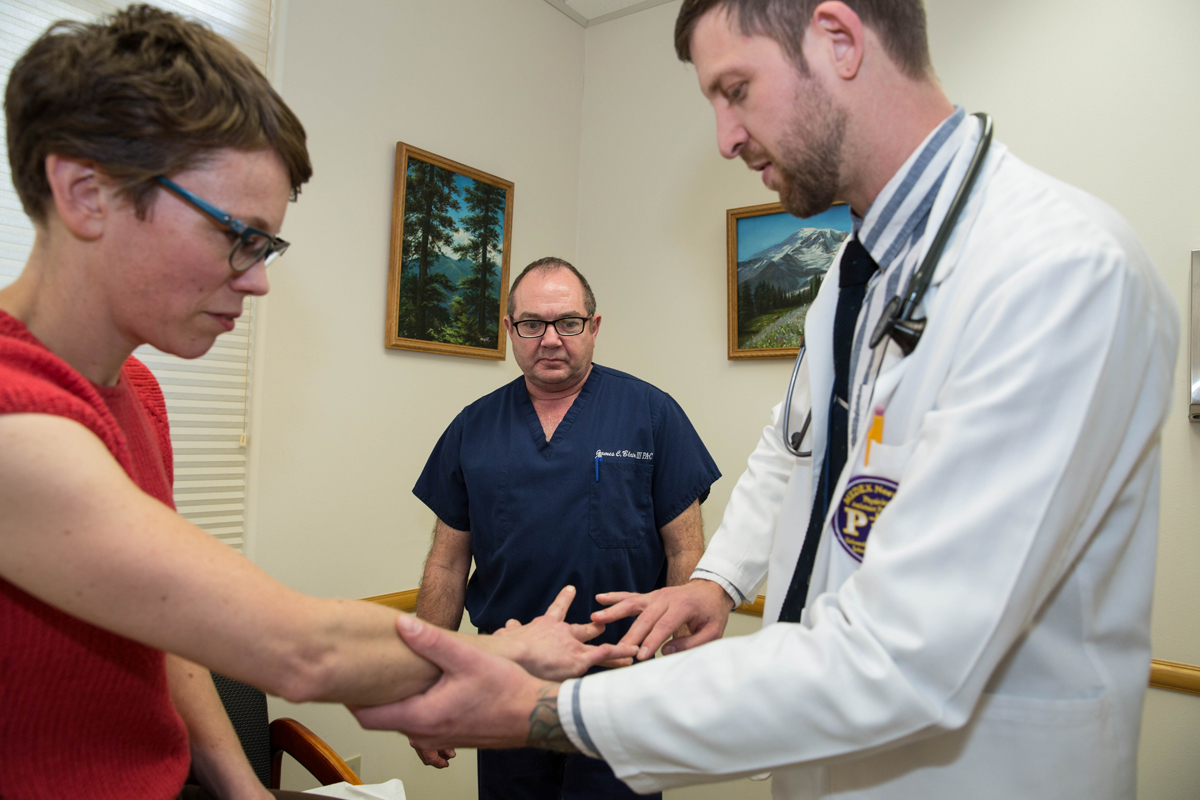
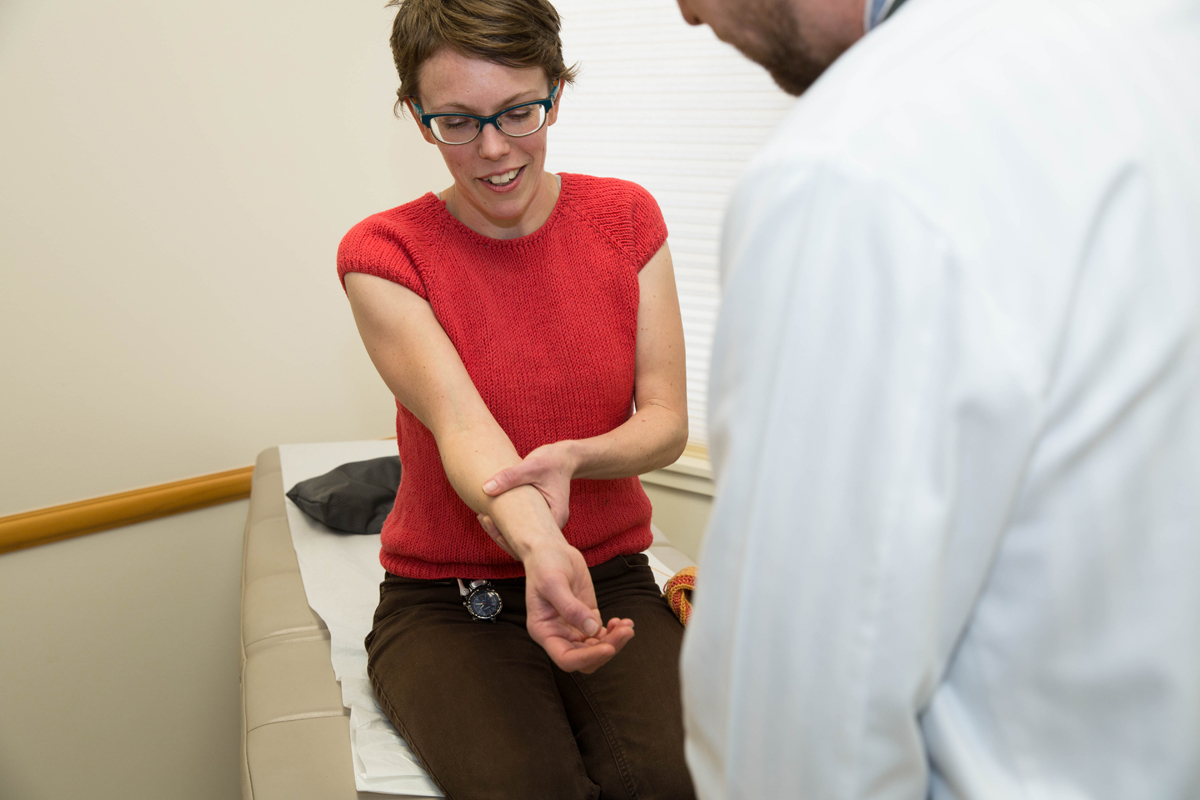
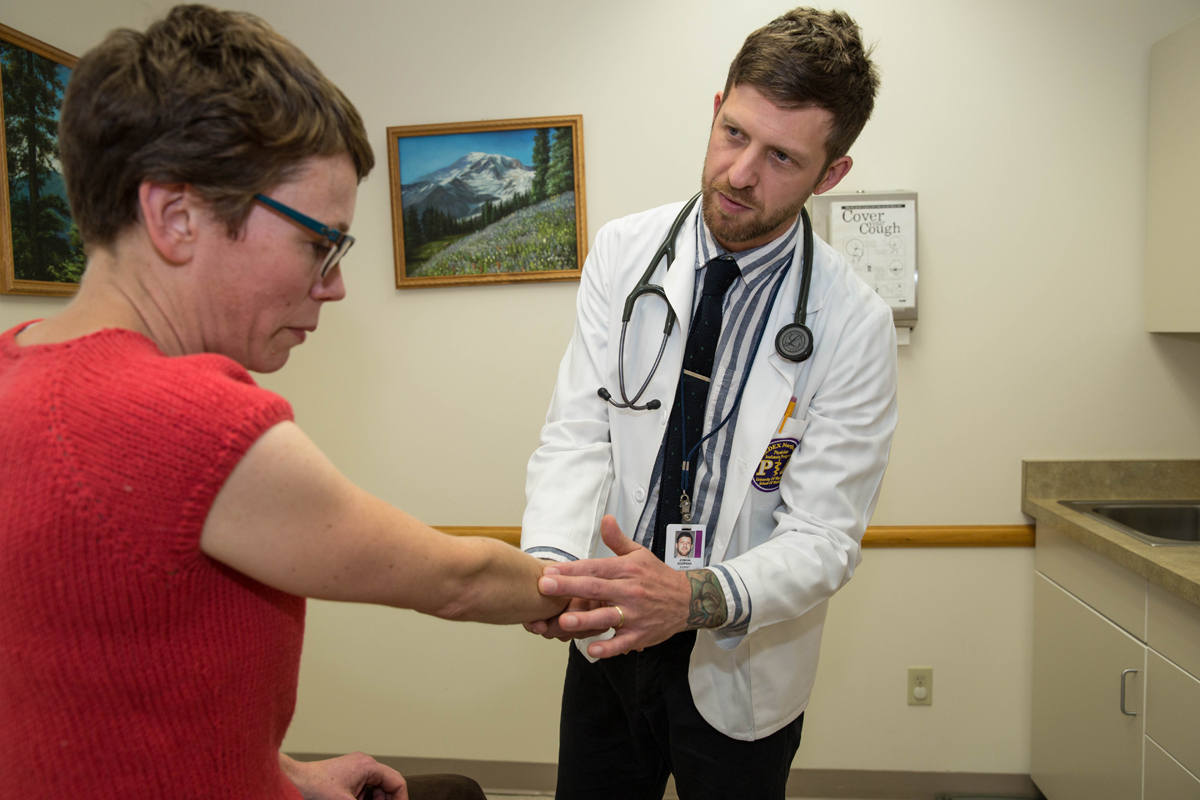
Our visit with Joshua Koopman takes place in Port Townsend, Washington during his family medicine preceptorship at Madrona Hill Urgent Care. He’s under the direction of Jim Blair, PA-C, himself a graduate of MEDEX Northwest from 1993. The MEDEX Northwest clinical curriculum gives emphasis to family medicine with a 4-month preceptorship, in addition to six 1-month specialty rotations including behavioral medicine, emergency medicine, general surgery, inpatient internal medicine, medically underserved populations and an elective.
Based on his earlier hospital experience, it’s not surprising to learn that Joshua has arranged for a cardiology elective. He’s located a California cardiac clinic that he hopes will give him the learning experience he needs to pass the national certification exam, or PANCE.
“It’s very hour-intensive,” he says. “They work a lot, but they give you housing there, they give you lunch and they apparently have teaching days. You know, where it’s, ‘Okay, today is Thursday. You’re going to spend your entire eight hours lecture learning.’ Even if I wasn’t interested in cardiology, having that rotation kind of cements the largest component of the PANCE, which seems pretty attractive to me.”
With graduation ahead in August of 2018, what kind of medical practice does Joshua foresee for himself?
“I really want to let the remainder of the clinical year inform what I do. I don’t want to close off doors to other specialties or avenues. But, you know, I like hospital settings so. I don’t like Monday through Friday, eight hours a day. Give me all my hours in three or four days, and then give me my breaks.”
Joshua has also done some shadowing on the cardiology unit at the UW Medical Center. “I love the way teaching hospitals have that stuff set up. It would be great if I could get into a setting like that, and be able to do two days surgery, one day in clinic. But I want to be open, too.”
Based on his overall experience of entering PA school, Joshua has some sage advice for those coming up behind him.
“It’s hard deciding to do something that is so competitive, especially when you don’t know if you’re going to get in. You have to commit a certain number of years and money and schooling, and it’s frightening. Is this actually going to work out?”
“People doubt their backgrounds a lot. The biggest thing for me was not to worry so much about whether I was going to get in, or how well I was doing. People stress out about their grades, and it takes your time and mind away from the essential thing. Like, ‘Okay, what is it that I have to study right now? What is this concept that I have to learn? How does it apply?’”

Joshua Koopman of MEDEX Seattle Class 50 and Jim Blair, PA-C of MEDEX Seattle Part-Time Class 1 from 1993.
“If you’re spending time thinking about what’s happening in the future, that’s less time you have to really you know your subject matter. And if you’re going to go to PA school, you should love the subject matter, because if you don’t, you’re going to wash out really fast. So, if you love it, then allow yourself the time to really be in the moment with it, and let the other things take care of themselves. Because if you do all that—if you’re passionate and you put in the time—you’ll do well. And I think eventually you’ll be able to find a good place in a program. Even if it’s not necessarily the one that you want, there are so many out there.”
“And since this is a process of life-long learning, accepting a novice perspective in the beginning will be paramount. This means you might feel dumb at times and identifying what you need may not always be possible. But it’s all applicable if you can keep an open mind and allow yourself some flexibility.”
We’re glad that Joshua found his “good place” at MEDEX Northwest, to master what is after all the art of medicine.