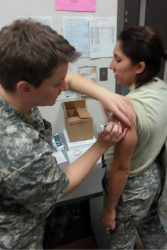
Alex Shaffer is working under Dr. Alan Thomas at Puget Sound Orthopedics in Lakewood, WA. “It’s fantastic,” he says. “We’re seeing lots of patients.” Dr. Thomas is an orthopedic surgeon specializing in the upper extremity: hand, arm, elbow.
There are two surgery days at the clinic.
“On Fridays, I get to scrub in and help out, doing whatever is needed. It’s great. I’m having a blast and I’m learning a lot. This is a really nurturing place.”
Alex is a clinical year PA student in MEDEX Northwest’s Seattle Class 51. Trained as a combat medic with the Oregon Army National Guard, he’s not a stranger to medicine. In the civilian world, a combat medic is the equivalent of an EMT. “During times of war, we’re practicing medicine through the US Army on the battlefield doing whatever it takes to save lives,” he says. “Otherwise we see people coming in with everything from coughs, colds, and sniffles to broken bones.”
Alex’s interest in medicine came early, well before becoming a combat medic.
“My mom finished nursing school when she was about my age,” Alex explains. Back in junior high school, Alex used to help his mother study by quizzing her with flashcards. “I think she was 42. She worked as a nurse for 20 years before medically retiring due to a back injury.”
From 2000 to 2003, Alex worked as a phlebotomist. But he always wanted to do more. And so, at the age of 30, he enlisted in the Oregon Army National Guard as a combat medic. He was supposed to be deployed to Afghanistan but got injured in training and required neck surgery.
“I have two titanium discs and four screws, C5 through C7,” he tells us.
There were two factors that prevented Alex from getting his physician assistant training through the military.
“I wasn’t qualified for the IPAP program because of my age and injuries,” he says. “At 42, I’m old and broken. I needed an age waiver, and I didn’t qualify to pass the physical to go into that program. I can try to commission after I graduate, which is my goal.”
On February 8th of this year, the US Army finally changed Alex’s gender marker to male. Born a female, Alex is officially, legally a male everywhere: birth certificate, driver’s license, military, everything. Going forward, he’ll use the male locker room and be housed with males.
“Unless you live under a rock, everybody knows what the word ‘transgender’ means,” he says.
But when Alex was growing up, he’d never heard the word.
“I was born in 1977 and knew I was different. When I was little, I always thought I was going to grow up and be a big boy like my dad.”
In conversations with his mother, she reports that she viewed him as different by age 4, and that she knew he was a boy by age 8.
“But we didn’t have a word for it, and you didn’t hear about it,” Alex says. “I mean, it was really taboo to even be gay at that point. And so, I didn’t know how to communicate how I was feeling, and my mom didn’t know what to do about it.”
All this made growing up in rural Oregon a struggle for Alex, with puberty an especially difficult time.
Finally, around age 20, he read something about people feeling that they were born in the wrong body. Alex’s response was, “Oh, that’s me. That’s what I am. That’s what’s going on.”
“It just clicked with me,” Alex says. “I did a lot of research, and realized that’s who I am.”
The 2013 American Psychiatric Association’s Diagnostic and Statistical Manual of Mental Disorders, 5th Edition – commonly referred to as the DSM-V – classifies this condition as gender disorder.
“At that time, you had to see a therapist for a full year before you could start hormone treatment.”
In his late 20s, Alex was living in Texas, then moved back to Oregon. He enlisted in the military.
“My thinking at the time was, ‘Well, I can have one dream or the other.’ So, I just kept hiding who I was except from my mother and a very few close friends.”
On June 30, 2016, Secretary of Defense Ash Carter announced that transgender individuals would be able to serve openly in the U.S. armed forces.
“Finally, I’m not living a lie anymore,” says Alex. “And I decided to be myself.”
Alex talked to his commanding officer to obtain permission. Her response was, “Yes, please. Go, be who you are.”
Alex’s family was very supportive through it all. He started taking testosterone on April 1st, 2016. “It’s the VA Endocrinology that gives me my hormone treatment,” he says. On August 21st, 2017 Alex had top surgery during his clinical year at MEDEX.
For his required Capstone Research Project, Alex chose to write on the challenges in healthcare for transgender people.
“You know, there is discrimination,” he says. “But a large part of it is just ignorance. Everybody thinks it’s really difficult to handle hormones when, in reality, managing insulin for a diabetic is much more complicated. There’s very little education about transgender care in medical school, PA school and among healthcare provider schools.” The focus of Alex’s capstone is primary care of a transgender patient.
Alex notes the lack of focus on trans healthcare issues in the current MEDEX curriculum.
“We got very little instruction about transgender healthcare,” he says. “Mostly, I would give the class my perspective as a patient. At least I can help there. I’d like to change that.”
 “You could have a patient come to you that needs their yearly physical, or they’re sick, and the fact that they’re transgender can play a significant part,” he says. “What if you have a man sitting in front of you that still has a cervix and is sexually active? They’re still going to need pap smears. Or you have a female that could have prostate cancer. We need to be more aware and realize that people are people and treat them for the body parts that they have. Yes, hormone therapy can change things like cardiovascular risk. We need more education.”
“You could have a patient come to you that needs their yearly physical, or they’re sick, and the fact that they’re transgender can play a significant part,” he says. “What if you have a man sitting in front of you that still has a cervix and is sexually active? They’re still going to need pap smears. Or you have a female that could have prostate cancer. We need to be more aware and realize that people are people and treat them for the body parts that they have. Yes, hormone therapy can change things like cardiovascular risk. We need more education.”
Alex believes that knowledge is power. “We’re not necessarily going to eliminate bias and discrimination. But the more we can educate people or put a face on things, the better we can overcome ignorance.”
Even within his own National Guard unit, Alex has seen changes since Secretary of Defense Carter’s announcement. With the official announcement in 2016, some soldiers pushed back, expressing concern about sharing shower facilities with transgender individuals. As a member of Oregon MEDCOM, a medical unit, Alex spoke out during one of the official educational sessions.
“It’s not about that,” Alex says. “I told them, ‘Hey, you know what? It’s not like anyone will be checking you out or flashing their genitals. We are more uncomfortable with those body parts than you are.’”
Within the Oregon National Guard, Alex has become the spokesperson on transgender issues. He consults with military providers on trans healthcare issues.
“I still take some flack,” he says. “I do encounter people that have an issue serving with me. But I just say, ‘You don’t have to be okay with who I am, just like I don’t have to be okay with who you are. We are required to respect each other’s rank, uniform, and work together.’ That’s all.”
Alex Shaffer will graduate with MEDEX Seattle Class 51 in the fall of 2019. Before that can occur, he’s got a 4-month family medicine preceptorship with Dr. Kirk Harris in Tumwater, WA. That will be followed by an inpatient trauma rotation at Legacy Emmanuel Hospital in Portland, OR.
“I’m coming full circle here because, when I totaled my Harley on September 3rd, I was a patient for two days at the same place,” he says. Alex will be learning from the same people who treated him when he had his motorcycle wreck. His final preceptor will be Jonathan VanHorn. “That’s Lieutenant Colonel VanHorn to me, because he’s in the Oregon National Guard as well and I’ve worked with him throughout the years.”
After graduation and certification, Alex looks forward to returning to his home state of Oregon and a job with the National Guard.
“Well, the military would just be part-time,” he says. “My ultimate goal is to find a good job in a small town in rural Oregon, buy some property, be close to my aging parents, help to take care of them, and adopt kids.”