[Skill Modules
>>
Neck & Veins Examination
>>
Teaching Tips
]
Teaching Tips: Neck Veins
General Points
- As with any physical sign, it is helpful to have the learner commit to an assessment before utilizing technology, such as radiography, ECG, or invasive monitoring.
- Talk aloud to describe the maneuver as it is being performed.
- To keep all participants interested, pose questions that learners can be thinking about until it is their turn to examine patients.
- Ask the patient's permission before reviewing the sign as a group. Summarize to the patient when the exam is completed.
- There are different way to approach the exam depending upon the level of the learner:
- A finding may be simply demonstrated, or
- A brief patient history may be given and the learner asked to demonstrate appropriate exam maneuvers, or
- Demonstrate various maneuvers to detect an abnormality (e.g., ascites), and ask learners about the value (sensitivity and specificity) of each exam maneuver.
- Historical points are fun and enhance interest in the exam.
back to top
JVP
- As teacher, start by simply localizing the internal jugular vein. When learners realize that the undulating movement distinguishes the jugular from the carotid arter, the vein will be quickly located.
- We recommend that teams on work rounds or attending rounds try to look at JVP on at least one patient every day, so that, by the end of the month, residents and students will have seen many patients with normal JVP and with abnormal findings.
- Practic identifying JVP in patients in whom the central pressure is known, i.e., those with central lines.
- JVP is most easily learned with the following:
Sinus rhythm
pulse <100
Respirations unlabored
- Occlusion of the jugular vein at the base of the neck will obliterate the venous pulsations, and the refilling by release of the vein may make the wave more prominent.
- Pearl: studies show that clinicians are more accurate in identifying tht jugular venous distention is present than quantifying the degree of elevation.
back to top
Jugular Venous Waveforms
NSR Wave Pattern
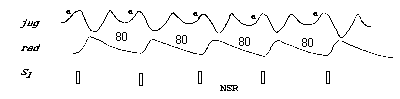
- As the diagram illustrates, localize the jugular waveform in relation to S1 and to the radial pulse.
- Xerox or trace the normal jugular venous pulse from a text example and highlight the area that represents systole. Carry this on a card and compare at the bedside to the patient's waveform (Sapira). For example:
normal wave
giant a wave with impaired y descent
cv merger wave
striking y descent wave
|
