[Skill Modules
>>
Pulmonary Examination
>>
Laboratory & Imaging
]
Laboratory & Imaging: Pulmonary
Analysis of pleural fluid requires several laboratory tests, particularly those to help distinguish "transudative" from "exudative" effusion. Tests on pleural fluid that are useful in the initial work-up of a pleural effusion include:
| Gross Appearance |
|
| Cell counts |
WBC with differential and PMN count RBCs |
| Total protein |
(calculate ratio with simultaneous serum protein) |
| LDH |
(calculate ratio with simultaneous serum LDH) |
| Glucose |
|
| Gram's stain and culture (bedside culture required) |
(if tuberculosis is suspected, peritoneal biopsy of higher yield than tubercuulosis smear adn culture |
| Cytology |
|
| Pleural fluid pH |
|
back to top
Pulmonary Function Tests
Pulmonary function tests (PFTs) are useful in a variety of clinical settings:
- Aid in diagnosis of underlying pulmonary disease
- Determine type of defect present (restrictive or obstructive)
- Quantify severity of disease and monitor progression over time
- Preoperative evaluation to assess fitness for surgery
- Bedside assessment of exacerbation of lung disease
- Determine injury from industrial hazards
Definitions of frequently used spirometry measures of lung function
Forced expiration (FEV)
The subject inspires maximally, and then exhales as hard and completely as possible. The volume of air exhaled in the first second is called FEV1 and the total volume exhaled is the forced vital capacity (FVC). Normally the FEV1 is about 80% of the FVC.
Vital capacity (VC)
The largest volume measured on complete exhalation after full inspiration.
Flow volume curves
The first small part of air exhaled in forced expiration is due to airway collapse. Subsequently flow is limited by airway compression and is determined by the elastic recoil force of the lung and airway resistance.
| Lung Volumes |
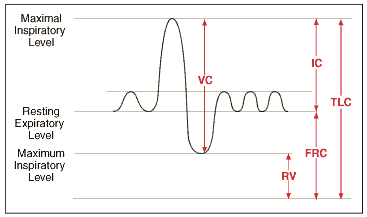 |
| VC |
Vital Capacity |
| TLC |
Total Lung Capacity |
| RV |
Residual Volumey |
| IC |
Inspiratory Capacity |
| FrC |
Functional Residual Capacity |
Two patterns can be distinguished by these measurements:
Restrictive lung disease (example: pulmonary fibrosis):
- Maximum flow rate is reduced, and total volume exhaled is reduced:
- Both FEV1 and FVC are reduced
- The ratio of FEV1/FVC is normal or increased
- Inspiration is limited by the reduced compliance of the lung or chest wall, or weakness of the inspiratory muscles
- Obstructive lung disease (examples: asthma, COPD)
- Total lung capacity is typically abnormally large but expiration ends prematurely (low flow rate in relation to lung volume):
- FEV1 is reduced much more than FVC
- Low FEV1/FVC ratio
- In obstructive airway disease due to asthma, this is due to increased muscle tone of the bronchi. In COPD, there is loss of radial traction from surrounding parenchyma. Other causes of obstruction include edema of bronchial walls or secretions within the airways.
- After bronchodilator therapy, obstructive changes on PFTs usually normalize with asthma but less so with COPD. Some COPD patients have a reversible or "reactive" component showing response to bronchodilators. (Note: Even if PFTs do not change, patients often are functionally better with bronchodilator therapy.)
Mixed patterns are frequently seen.
(Source: Gold)
|
