"What happens to my data?" "What are researchers finding based on our study participation?"

UW ADRC research participants make it possible for scientists to discover fundamental mechanisms of Alzheimer's disease and related conditions and contribute to knowledge that will lead to therapeutics and prevention measures.
Every day, investigators publish studies that rely on biological samples or clinical data generously donated by those enrolled in the UW ADRC Clinical Core longitudinal study and the Adult Changes in Thought Study (ACT). The UW ADRC considers your contribution of data and specimens, including brain autopsies, to be the ultimate gift to future generations. This research was made possible in part by funding from the National Institute on Aging, grant AG066509.
For these studies, researchers used data from participants in the UW ADRC Clinical Core, with gratitude.
Improving diagnostic accuracy of cognitive testing for Latinx/o/a in the United States

Marquine MJ, et al. Alzheimer’s & dementia: the journal of the Alzheimer’s Association, 2023
A team of researchers from Alzheimer’s Disease Research Centers (ADRCs) across the country have taken an important step toward improving the accuracy of memory and thinking testing among Spanish- and English-speaking Latinos in the United States.
All ADRCs use a set of the same memory and thinking tests to assess the cognitive functioning of participants enrolled in their memory study, and to track any changes over time. This standard group of tests is designed to detect cognitive impairment. But because most participants in ADRC studies are non-Hispanic white, it is uncertain whether the test results mean the same thing for people in historically minoritized groups.
In the study, 437 healthy Latino adults, recruited from across 33 ADRCs, completed the test in their preferred language. The researchers then used the scores in mathematic models that found associations of age, years of formal education, and sex with scores on the cognitive tests. They were able to see patterns within these groupings by demographic characteristics. For example, more years of education were linked to better test scores among Spanish-speakers.
Other researchers will be able to use these new data to ensure the test accurately reflects cognitive ability among Latinos enrolled in ADRCs. Such efforts are needed to address disparities in Alzheimer’s disease.
Understanding mid-life obesity and dementia risk

Batabyal, RA et al. Int. Journal of molecular sciences, 2023
Research shows that being severely overweight or obese in middle age is associated with a three-fold increased risk of dementia 30 years later.
To better understand the link between midlife obesity and the increased risk of Alzheimer’s disease, a team of researchers studied samples of blood and cerebrospinal fluid of 18 ADRC research participants living with Alzheimer’s disease, as well as 14 healthy control subjects. In these fluid samples, the team looked for exosomes, or cellular vesicles that carry key proteins and genetic information from cell to cell. They were able to isolate the exosomes specifically released from fat cells, and then they analyzed the molecular cargo inside.
In the samples from participants with Alzheimer’s disease, they found evidence that genetic messages carried by fat-cell derived exosomes affect the working of a key pathway involved in the health of neurons, learning, and memory. These findings suggest a way that midlife obesity can increase the risk of Alzheimer’s disease and identify a treatment target.
Finding Clues to Alzheimer’s in the Brain’s Immune Cells
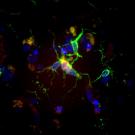
Image courtesy of Alexandra Cochoit, UW Neurology. See bigger
Prater, KE et al. Nature aging, 2023
Microglia are a type of cell that play very important roles in our brain health. They have a diversity of jobs, including maintaining normal brain function, fighting infections, and cleaning up and disposing of dead cells and waste. Research suggests that in people with Alzheimer’s disease pathology in their brains, some microglia react too strongly, causing so much inflammation that the response drives the disease, rather than preventing it.
An ADRC research team used brain autopsy samples from 22 ADRC research participants to learn more about the groups of microglia that respond to Alzheimer’s disease. To do so, they studied the microglia gene expression, or the messages that get turned into proteins for use in the cell to perform in their specific job.
In a new paper, the team describes three different groups of microglia that have not been seen before in the human brain. All three groups showed signs of being involved in waste disposal duties. But one of these groups appeared more often in brains of people who had Alzheimer’s disease during life. The gene expression of these microglia also showed signs of inflammatory activity. This finding is a new clue to how microglia respond to Alzheimer’s pathology. They also looked at a population of microglia known to help send messages between cells, and they found a subgroup only found in Alzheimer’s disease brain tissue.
“Instead of using medications to treat the whole immune cell population, we can now target just the type of microglia that are harmful,” says lead author Katherine Prater, PhD. The team is now positioned to study microglia’s role in Alzheimer’s disease, with more precision than ever before.
Genetics of Alzheimer's Disease
Course M et al. Aberrant splicing of PSEN2, but not PSEN1, in individuals with sporadic Alzheimer's disease. Course MM et al. Brain. August, 2022

NIH
Pathogenic gene variants in PSEN1 and PSEN2 are rare causes of familial Alzheimer’s disease. UW researchers now have reason to think that these genes also hold clues to cases of the more common late-onset ‘sporadic’ Alzheimer’s disease. Recent work from a UW team, including UW ADRC researchers, found that age-related changes in the way PSEN2 generates transcripts (instructions for making proteins) might be involved in sporadic Alzheimer’s risk in the general population.
The team has since worked to identify these flawed recipes for proteins in Alzheimer’s pathology. “This project is exciting,” says study author Paul Valdmanis, assistant professor of medical genetics in the UW Department of Medicine, because “we could provide insight into why individuals develop Alzheimer’s disease without a family history of disease.”
In a new study published in Brain, the team characterized novel PSEN1 and PSEN2 transcripts in samples from cases of both familial and sporadic Alzheimer’s disease from the UW ADRC and compared these against healthy controls from the ACT Study. They leveraged PacBio Iso-Seq—a third-generation sequencing method for obtaining long reads of transcripts.
The team found certain abnormal splice products of PSEN2 only in late-onset sporadic Alzheimer’s disease samples. This finding suggests that genetic transcript differences in PSEN2 may play a role in Alzheimer’s disease in the general population. The researchers see this finding as a first step towards discovering new ways to preserve genetic function as a possible future treatment.
Increasing the Value of Data from Memory Testing
Mukherjee J et al Cognitive domain harmonization and co-calibration in studies of older adults. Mukherjee S, et al. Neuropsychology, Aug. 2022.

UW Medicine/Getty
In large, long-running studies of older adults, such as the Adult Changes in Thought (ACT) Study (participants = 5,546) and the Rush Memory and Aging Project (participants = 2,163), participants attend regular research visits over time and undergo different procedures including tests of thinking and memory. These studies generate large amounts of data that researchers can use to find associations between lifestyle or genetic factors and late-life cognitive functioning and impairment.
However, the specific types of memory and thinking tests that researchers used tend to vary from study to study. This lack of standardization across studies makes it difficult for researchers to compare individual results when using data pooled from multiple studies.
In what Paul Crane, MD, MPH, professor of medicine at the UW School of Medicine, calls a ‘Hello World” methods paper, a UW team shares the results of a major effort to make it easier for researchers to leverage data from multiple studies of older adults. They have succeeded in taking the cognitive test scores from 10 different studies and calibrating them according to the same metric.
These calibrated test scores for 10 different study datasets have many benefits to the Alzheimer’s field. A researcher can focus on their important scientific question without having to spend as much valuable time manipulating statistics. “Our science is really benefiting a lot from the recent moves towards data sharing and data availability,’ says Crane. “Our group is doing the work to make it so that those shared data are amenable to quick scientific analyses of relationships between cognition and whatever else is of interest, across multiple different datasets—and without anyone else needing to worry about the details that we worry about.”
The team is currently working to generate these co-calibrated memory scores for datasets from the UW ADRC Clinical Core, to make their participants’ data even more easily accessible to other researchers across the country. Crane thinks that this larger data harmonization approach will ultimately lead to more confidence in scientific results in the Alzheimer’s field because researchers can check if an association found in one study can be confirmed in a different dataset.
Advancing Blood Tests for Alzheimer's Disease
Shea D et al. SOBA: Development and testing of a soluble oligomer binding assay for detection of amyloidogenic toxic oligomers. Shea et al. Proceedings of the National Academy of Sciences USA, December 2022

In the earliest stages of Alzheimer’s disease, the brain forms toxic aggregates, called oligomers, of the protein amyloid beta. These oligomers can start to form more than a decade before symptoms begin to present and before any other known disease markers develop. The ability to detect these oligomers could help medical providers detect and diagnose Alzheimer’s disease much earlier, impacting course of treatment and staving off irreversible progression.
An NIH-funded research team, led by Valerie Daggett, professor of bioengineering at the University of Washington, in collaboration with ADRC researchers, created a synthetic molecule capable of selectively binding to toxic forms of amyloid beta, but not its non-toxic counterparts. From this molecule, called AP193, they developed an assay method to detect toxic amyloid beta in patients’ blood. This assay, called the soluble oligomer-binding assay (SOBA), was used on nearly 400 banked human blood plasma samples from UW ADRC research participants. These participants were categorized into the following groups: a control group of individuals with no known cognitive impairment, a group with mild cognitive impairment (or MCI), a group with Alzheimer’s disease, and a group carrying other forms of cognitive impairment.
SOBA ultimately detected the presence of toxic oligomers in 52 out of 53 people in the Alzheimer’s disease and MCI groups. As expected, the blood test did not detect oligomers in most of the samples of control subjects who had no cognitive impairment. However, SOBA detected oligomers in 11 controls, and 10 of these positive samples came from people who later developed MCI. This finding shows that the SOBA test detected the toxic oligomers of amyloid beta before Alzheimer’s symptoms appeared. The researchers suggest that SOBA could form the basis for early diagnostic tests.
“We believe that SOBA could aid in identifying individuals at risk or incubating the disease,” Daggett says, “as well as serve as a readout of therapeutic efficacy to aid in development of early treatments for Alzheimer’s disease.” Daggett has a startup company working on this promising platform for early diagnosis and treatment of Alzheimer’s. Adapted from NIH Research Matters
Better Support for Caregivers of Loved Ones with Lewy Body Dementia
O. Zaslavsky et al. Virtual Intervention for Caregivers of Persons With Lewy Body Dementia: Pilot Quasi-Experimental Single-Arm Study. Zaslavsky et al. JMIR Formative Research, July 2022
A team of researchers from the UW School of Nursing and UW Medicine recently completed a pilot evaluation of a digital intervention designed to help support caregivers of people with Lewy body dementia. The primary goal of this intervention, called Virtual Online Communities for Aging Life Experience-Lewy Body Dementia (or VOCALE-LBD), is to promote resilience and reduce stress in this vital population.
The Lewy body dementias, a term referring to both dementia with Lewy bodies and Parkinson’s disease dementia, are the second most common type of dementia in older adults. People with Lewy body disease often develop disruptive behaviors and sleep problems that can make caregiving particularly challenging. Compared to other types of dementia, caregivers of people with Lewy body dementia tend to report relatively higher levels of stress and more severe depressive symptoms.
With help from the UW ADRC, the research team recruited 15 family caregivers of people living with Lewy body dementia to participate. VOCALE-LBD is an 8-week interventional program conducted over a web-based discussion platform (that is moderated by study staff) and designed to enable peer-to-peer support, education, training, and problem-solving skill practice.
In the study, many caregivers reported that participation in VOCALE-LBD helped them better understand the disease, feel more confident in dealing with difficult behaviors, and improve their ability to care for their loved one. If validated in future studies, the intervention could become a valuable resource for caregivers, helping them to develop crucial inter-personal support networks without having to leave their homes. The team is now looking for informal caregivers of people with Lewy body dementia to participate in the next step of this project: conducting virtual focus groups and usability testing sessions. If you are interested in learning more or participating, please visit this VOCALE-LBD webpage.



